| Journal of Medical Cases, ISSN 1923-4155 print, 1923-4163 online, Open Access |
| Article copyright, the authors; Journal compilation copyright, J Med Cases and Elmer Press Inc |
| Journal website https://www.journalmc.org |
Case Report
Volume 14, Number 11, November 2023, pages 378-386
Clinical Evolution After Administering Antivenom in Patients With Loxoscelism
Omar Azuara-Antonioa, b, Mario I. Ortizb, c , Karla D. Jimenez-Oliverb, Luis E. Hernandez-Cruza, Gamaliel Rivero-Verasa, Luz Hernandez-Ramireza
aHospital General de Pachuca, Pachuca, Hidalgo, C.P. 42070, Mexico
bArea Academica de Medicina, Instituto de Ciencias de la Salud, Universidad Autonoma del Estado de Hidalgo, Pachuca de Soto, Hidalgo, C.P. 42090, Mexico
cCorresponding Author: Mario I. Ortiz, Area Academica de Medicina del Instituto de Ciencias de la Salud, Universidad Autonoma del Estado de Hidalgo, Col. Doctores, Pachuca, Hgo 42090, Mexico
Manuscript submitted October 4, 2023, accepted November 7, 2023, published online November 23, 2023
Short title: Treating Loxoscelism Using Antivenom
doi: https://doi.org/10.14740/jmc4163
| Abstract | ▴Top |
Spiders are the most numerous arthropods of the arachnid class. More than 45 thousand species of spiders have been identified, and only a few are dangerous to humans. Among them, the “violin spider” or “brown spider” of the genus Loxosceles (family Sicariidae) has a worldwide distribution, and its bite can cause loxoscelism. Initial treatment of a Loxosceles spider bite includes application of local cold, rest, elevation of the extremity if possible, and systemic pharmacotherapy with antihistamines, corticosteroids, antibiotics, polymorphonuclear inhibitors, and analgesics or nonsteroidal anti-inflammatory drugs. During cutaneous or systemic loxoscelism, administration of Loxosceles antivenom (immunoglobulin (Ig)G F(ab’)2 fragments) may be indicated to prevent progression to severe systemic phases. In this manuscript, we present three cases of patients with loxoscelism treated with the fabotherapeutic Reclusmyn®, developed and manufactured in Mexico. Two patients had a satisfactory outcome without severe skin or systemic damage. Only one patient with loxoscelism, despite early initiation of antivenom, had extensive skin lesions that healed satisfactorily, leaving only a non-disabling scar. Due to the global presence of this clinical problem, further studies are needed to establish local and general guidelines for the treatment and prevention of loxoscelism. This will allow health professionals to provide more efficient and higher quality medical care and feel supported in their decisions.
Keywords: Loxoscelism; Bite; Loxosceles spider; Antivenom; Fabotherapeutic
| Introduction | ▴Top |
Loxoscelism is a state of envenomation characterized by a series of clinical manifestations caused by the bite of the Loxosceles spider, commonly known as the “fiddler”, “brown”, “corner” or “brown recluse”. These manifestations can be divided into cutaneous and systemic forms, with the cutaneous presentation being more common, with local signs at the site of the lesion, as opposed to systemic loxoscelism, which is associated with serious complications and even death [1, 2]. There are 143 species of Loxosceles spiders described around the world, identifying approximately 122 species in the Americas and 40 species distributed throughout of Mexico. The main species in Mexico are Loxosceles reclusa and Loxosceles rufescens. Four species in the state of Hidalgo from Mexico have been described (Loxosceles jaca, Loxosceles nahuana, Loxosceles tenango, Loxosceles tolantongo) [3-6]. There is no record of the exact number of accidents caused by Loxosceles species in Mexico, but it has been reported that 11% of animal envenomations are caused by arachnids [6]. Approximately 85% of Loxosceles bites produce only cutaneous manifestations caused by its venom [4-6].
In the systemic form, the venom can primarily affect organs such as the liver, kidneys, heart, skin, and blood tissues. In addition to phospholipase D (PLD) in the Loxosceles venom, other enzymes such as hyaluronidases and metalloproteases may promote the spread of other toxins to nearby tissues and the systemic circulation [1, 7]. An inoculation of approximately 4 µL of venom is required to produce intoxication, but the intensity of the reaction is affected by the susceptibility of the victim and the amount of venom inoculated, thus producing the different forms of presentation, local or systemic [1, 7].
Hemolysis, thrombocytopenia, and signs of disseminated intravascular coagulation (DIC) may occur, resulting in severe endothelial damage, producing areas of inflammation that progress to areas of necrosis of varying extent due to thrombosis [8-10]. Endothelial damage may increase, resulting in prolonged hypotension, lesions of various mucous membranes, glomerulonephritis, pulmonary lesions leading to respiratory failure, and central nervous system lesions, mainly vasculitis [8-10].
The therapeutic approach to loxoscelism depends on the type of envenomation (cutaneous or systemic), the timing of the bite and the presentation to health services, the clinical evolution of the patient and the probable complications. In cutaneous or systemic loxoscelism, administration of anti-Loxosceles serum (F(ab’)2 fragments of immunoglobulin (Ig)G) may be indicated to prevent progression to the severe systemic phases [11-14]. However, if loxoscelism does not progress to a severe or systemic form, only the skin lesion is treated until complete healing and scarring occurs (which may take weeks or months) [11-14]. The main purpose of this manuscript is to present three clinical cases of patients with loxoscelism treated with the fabotherapeutic Reclusmyn®, a drug developed and manufactured in Mexico.
| Case Reports | ▴Top |
Case 1
Investigations
A 14-year-old female, high school student, with no relevant medical history, who reported a spider bite on the right pelvic limb while in the backyard of her home, manifested by pruritus and burning pain of increasing intensity, for which she presented to the emergency department approximately 40 min after the bite. On physical examination, she was afebrile (36.8 °C), with a heart rate of 90 beats per minute, a respiratory rate of 24 breaths per minute, and a blood pressure of 110/69 mm Hg. The patient also had nausea. She vomited three times and had abdominal cramps and colicky abdominal pain. Examination revealed a lesion on the posterior aspect of the right thigh, in the region of the biceps cruris, with edema, erythema, and a blue-gray halo with irregular borders, measuring approximately 49 cm in diameter (Fig. 1), and painful to palpation (9/10 on the Visual Analogue Scale (VAS)). No changes were noted on follow-up. Subsequently, laboratory tests showed a slight increase in creatinine levels on the first and second days of hospitalization (1.24 and 1.2 mg/dL, respectively). On the third day of follow-up, the patient presented with leukocytosis (17.4 × 103/µL) and microalbuminuria (150 mg/24 h).
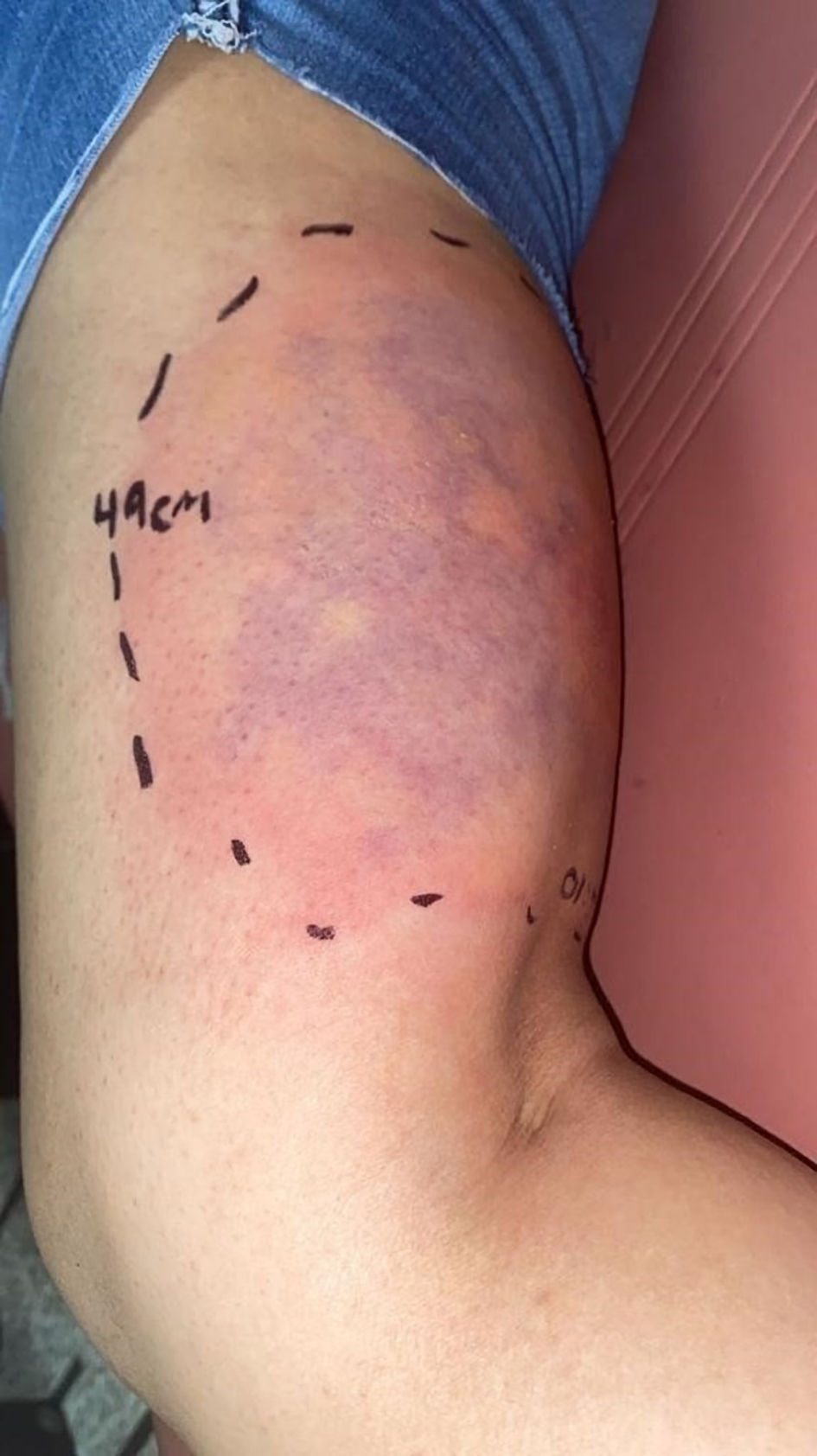 Click for large image | Figure 1. Lesion located on the right pelvic limb, with edema, erythema, blue-gray halo, irregular margins, with an approximate diameter of 49 cm. |
Diagnosis
The patient was evaluated by the Toxicology Service, which established the diagnosis of confirmed systemic or visceral-cutaneous loxoscelism based on the characteristic clinical picture and the fact that the patient had the arachnid that caused the poisoning (Fig. 2).
 Click for large image | Figure 2. Arachnid of the genus Loxosceles presented by the patient. |
Treatment
The patient was admitted to the hospital upon arrival at the emergency department. According to the history of the spider bite, the presentation of the image of the specimen involved (Fig. 2, compatible with a Loxosceles spider) and the evolution of the patient, it was decided to start treatment with the antivenom. Five vials of Reclusmyn® (polyvalent anti-Loxosceles fabotherapeutic) were indicated: two vials were administered 3.5 h after the attack, two vials 8 h after the bite, and one vial 2 days later. During hospitalization, the patient received crystalloid fluids based on 0.9% NaCl solution 1,000 mL every 8 h for 2 days. Subsequently, 1,000 mL of 0.9% saline was adjusted for 12 h. In addition to phototherapy, ceftriaxone 1 g daily (for 5 days), a single dose of methylprednisolone 30 mg, and ketorolac 0.5 mg/kg every 8 h (for 2 days) were started.
Follow-up and outcomes
During hospitalization, the patient presented oliguria and reflex tachycardia, establishing low cardiac output, so it was decided to start diuretic treatment (furosemide 30 mg intravenous (IV) every 12 h), in addition to IV administration of dobutamine and dopamine with weaning from it, continuing with ceftriaxone. Five days after the attack, there was a decrease in erythema and edema in the lesion, in which the formation of vesicles with serohematous content began, with subsequent rupture on day 12, initiating the formation of the necrotic ulcer (Figs. 3, 4).
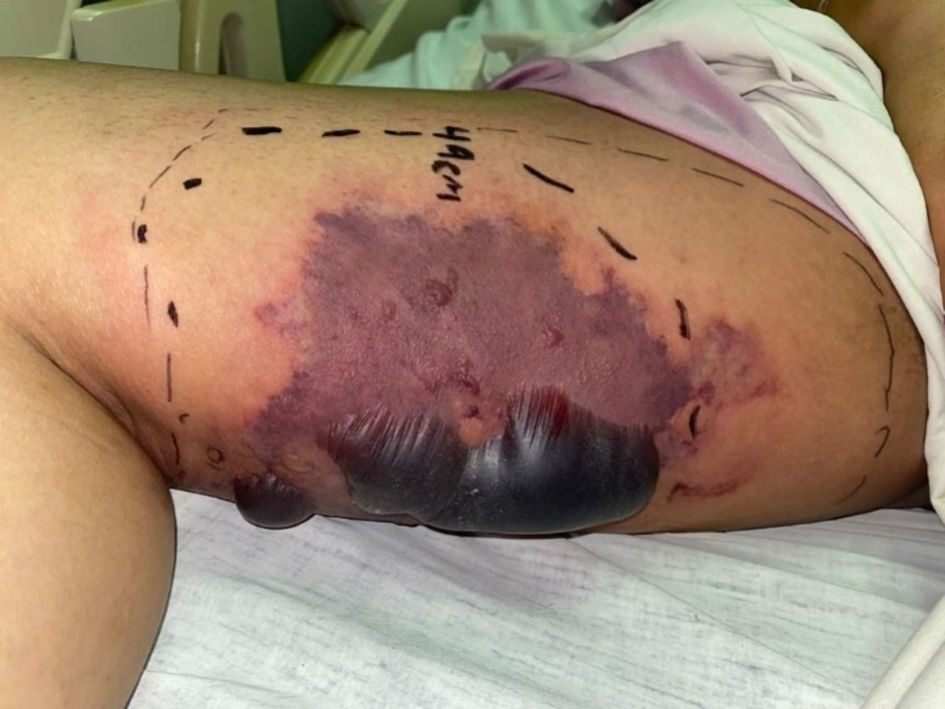 Click for large image | Figure 3. Decrease of erythema in the lesion, consolidation of liveloid plaque, and formation of vesicles with serohematous content. |
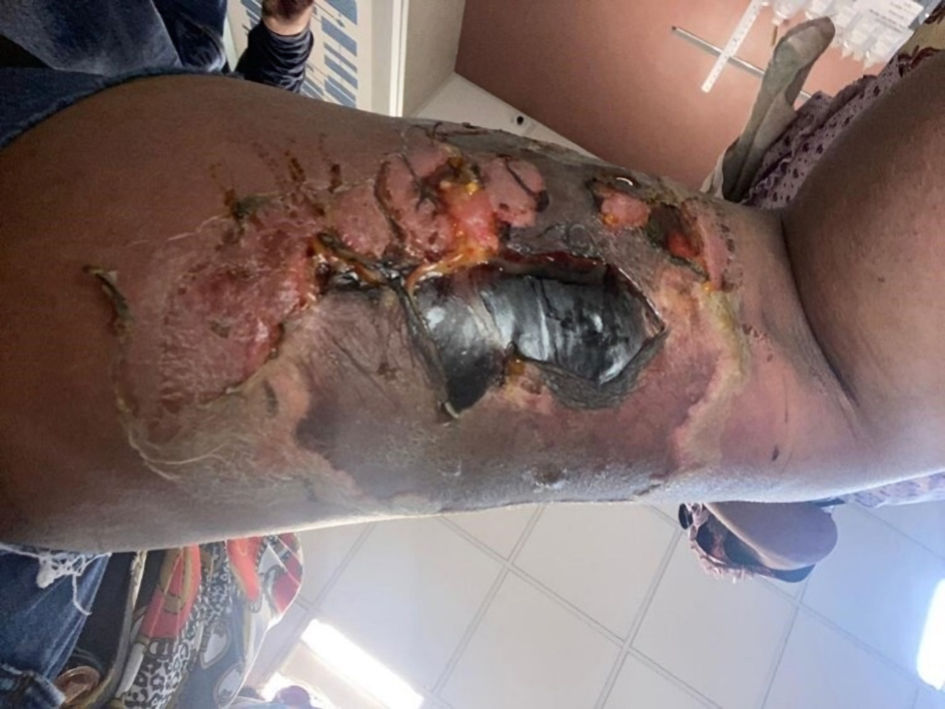 Click for large image | Figure 4. Rupture of the vesicles and desquamation of the dermis. |
Seven days after the bite, mechanical cleansing and debridement of the wound was performed (Fig. 5). On the eighth day after the spider bite, the patient demonstrated preserved renal function and adequate urine flow, so it was decided to discharge the patient for outpatient management. The patient attended the outpatient clinic once a week for wound checks. Forty-nine days after the spider bite, an autograft was placed over the wound without complications, and the patient was discharged at the end of the procedure. The lesion showed a favorable evolution with complete healing in 2 months, leaving a residual atrophic scar (Fig. 6). From the specimen presented by the patient, which was captured after the bite, it was concluded that it was an arachnid of the genus Loxosceles (Fig. 2).
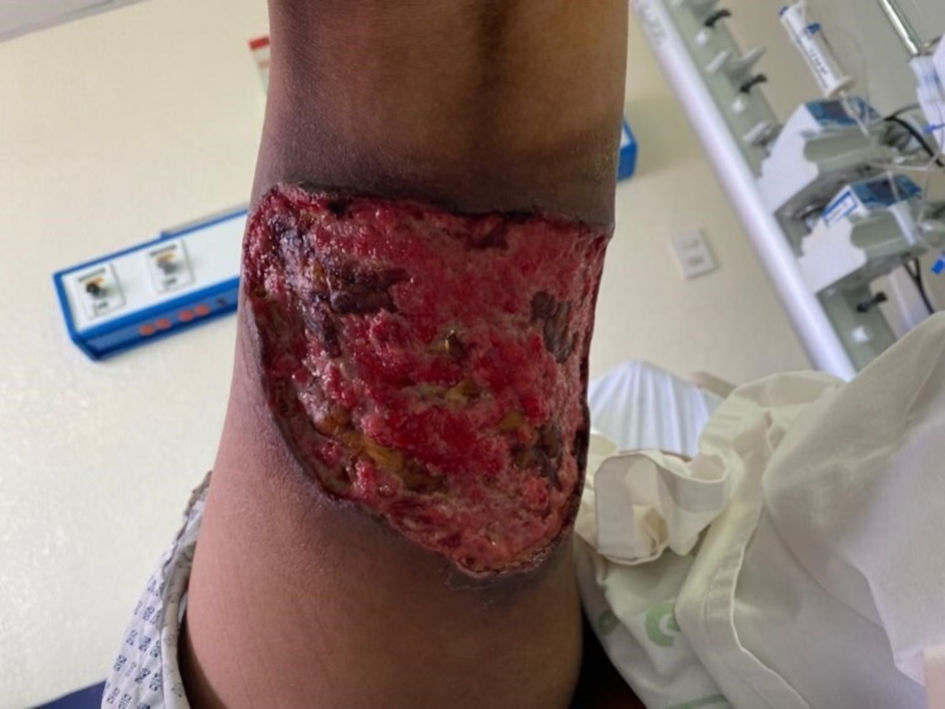 Click for large image | Figure 5. Lesion in the right pelvic limb after surgical lavage and debridement, with irregular edges, hyperpigmented, surrounding vitalized tissue. |
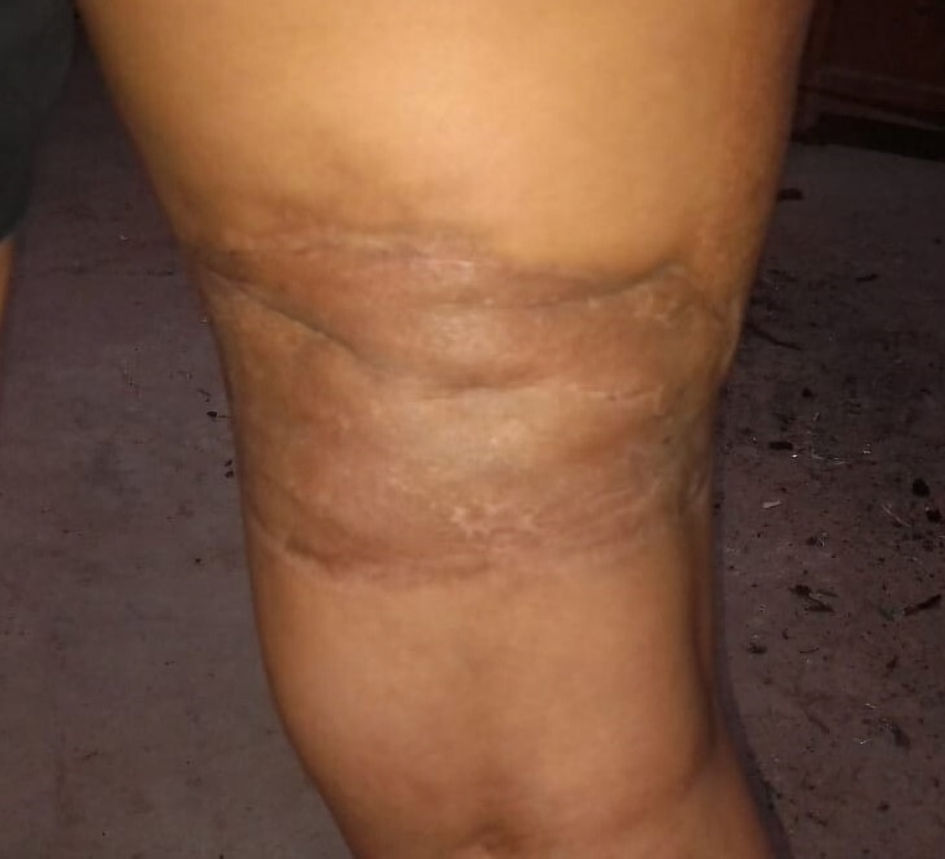 Click for large image | Figure 6. Complete resolution of the lesion 2 months after the attack, with residual scarring. |
Case 2
Investigations
A 23-year-old male university student presented to the emergency department with a circumscribed lesion of necrotic characteristics with serohematous contents, located on the left upper extremity, 4 cm in diameter, painful on palpation. The patient reported that his present condition began 6 days before, mentioning that he only felt pain in his arm due to a probable sting or bite, without identifying the cause. On the second day after the bite on the upper extremity, the patient reported pain, erythema, and inflammation at the site of the injury and mild general discomfort. For this reason, the patient decided to go to a private doctor’s office, where he was prescribed clindamycin, diclofenac, naproxen, hydrocortisone, and methylprednisolone (without specifying the doses). From the third to the fifth day after the bite, the patient reports worsening symptoms, so on the sixth day he decides to go to the emergency department. As an important clinical antecedent, the patient reported a history of testicular cancer (seminoma), which was treated with chemotherapy, and he was currently in complete remission 1 month prior to the current illness.
On physical examination, the patient was afebrile (36.5 °C), heart rate of 88 beats per minute, respiratory rate of 20 breaths per minute, blood pressure of 100/80 mm Hg, nausea, vomiting four times, colicky abdominal pain, muscle spasms localized in the abdomen and lower extremities. On inspection, a lesion was found in the proximal third of the anterior surface of the right forearm, with erythematous maculopapular characteristics, with areas of necrosis, circumscribed, with irregular borders, with a white halo 3.5 cm in diameter, with pain on palpation and movement (9/10 on the VAS) (Fig. 7). No changes were noted on further physical examination. During his hospitalization, the patient presented with acute kidney injury (creatinine of 2.71 mg/dL) and severe thrombocytopenia (lowest reported level of 5,000 platelets per microliter on the second day of hospitalization).
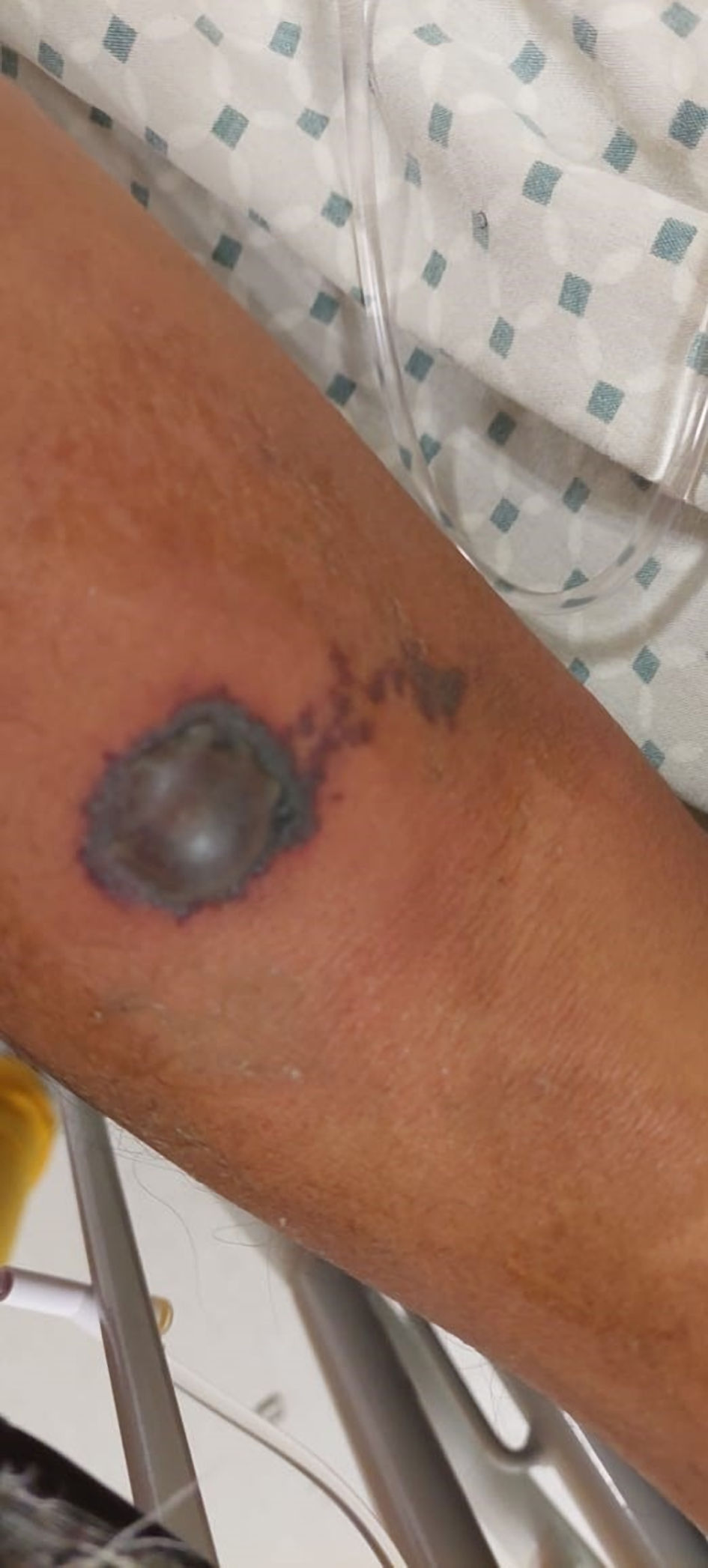 Click for large image | Figure 7. The skin lesion located on the right thoracic limb, with erythematous maculopapular characteristics, with serohematous content, irregular borders, with a white halo, together with a small diffuse liveloid plaque. |
Diagnosis
The patient was evaluated by the Toxicology Service, which made the diagnosis of probable systemic or visceral-cutaneous loxoscelism because the patient did not provide the specimen that caused the intoxication, so it was not classified as a confirmed case.
Treatment
According to the history of the bite on the left upper extremity, the characteristics of the skin lesion and the clinical evolution of the patient, it was decided to start treatment with antivenom. The use of four vials of Reclusmyn® (polyvalent anti-Loxosceles fabotherapeutic) was indicated, with two vials administered 10 h after admission and two more 24 h later, along with pain control with acetaminophen 1 g for 4 days and omeprazole 40 mg for 3 days. After fabotherapic treatment, the erythema and pain in the lesion decreased. Due to severe thrombocytopenia and acute kidney injury, it was decided to start treatment with crystalloids and transfuse only a platelet pool.
Follow-up and outcomes
The wound continued to progress favorably, and on day 11 after the bite, showed an ulcer with irregular borders, hyperpigmented, surrounding vitalized tissue with fibrin formation (Fig. 8). After 6 days of hospitalization, it was decided to discharge the patient definitively. The patient demonstrated preserved renal function (creatinine level of 1.23 mg/dL) and adequate urine flow, and outpatient follow-up visits were scheduled every 7 days to evaluate the wound. Ultimately, the lesion showed a favorable evolution with complete healing in 4 weeks with a residual scar.
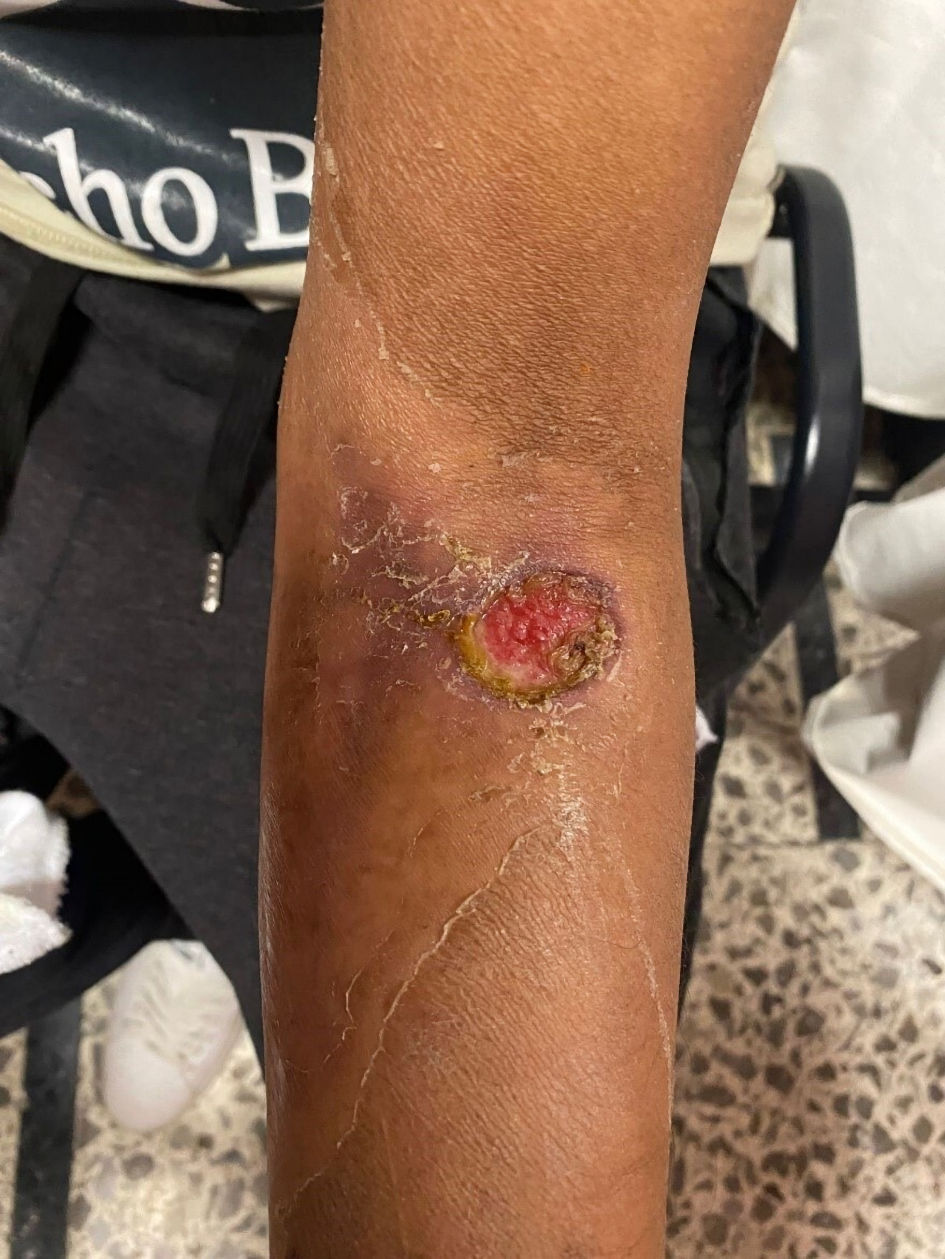 Click for large image | Figure 8. Ulcer with irregular borders, hyperpigmented, surrounded by vitalized tissue with fibrin formation after fabotherapeutic administration. |
Case 3
Investigations
A 20-year-old woman employed in a pharmacy with no relevant medical history reported a biting sensation in the left pelvic limb during cleaning at work, with pain and dysesthesia and an erythematous lesion. The patient then went to a private physician’s office, where she was prescribed a single dose of fexofenadine (120 mg). However, the patient did not perceive any improvement in the clinical picture, coupled with the appearance of a blister, increased pain, and erythematous area, then she decided to go to the emergency department of the hospital for evaluation about 5 h after the attack. On physical examination, the patient was afebrile (36.5 °C), heart rate of 88 beats per minute, respiratory rate of 20 breaths per minute, blood pressure of 110/70 mm Hg, and denying concomitant systemic symptoms. A maculopapular lesion with a central necrotic area and perilesional erythema with irregular borders was found on the left lower extremity, in the region of the middle third of the medial tibia, measuring 8 - 15 cm (Fig. 9) and painful to palpation (9/10 on the VAS). No other changes were noted on further examination. The patient reported nausea and vomiting on two separate occasions. Laboratory tests were carried out and the values were within the normal limits for the sex and age of the patient.
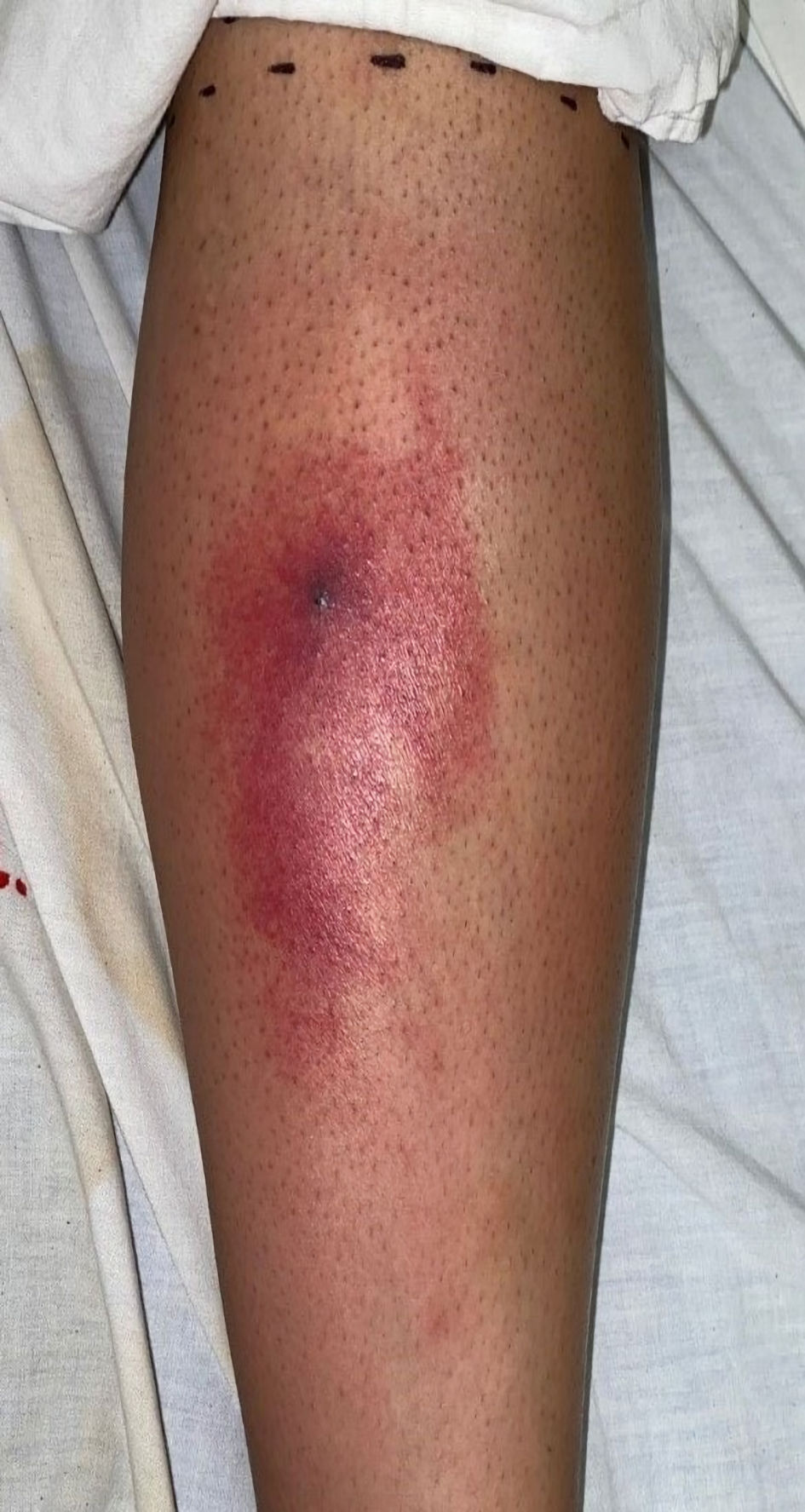 Click for large image | Figure 9. The lesion on the left lower extremity, in the area of the middle third of the medial tibia, of maculopapular type with a central necrotic area, with the presence of erythema with irregular borders. |
Diagnosis
The patient was evaluated by the Toxicology Service, which made a diagnosis of probable cutaneous loxoscelism because the patient did not provide the specimen that caused the intoxication, so it was not classified as a confirmed case.
Treatment
Based on the established diagnosis, treatment with acetaminophen, omeprazole, and ondansetron was indicated. In addition, four vials of Reclusmyn® (polyvalent anti-Loxosceles fabotherapeutic) were administered, starting with one vial 22 h after the attack, one vial 48 h after the attack, and two vials 72 h after the bite.
Follow-up and outcomes
The patient reported a decrease in pain, erythema, and dysesthesia following fabotherapy. The patient continued to tolerate the oral route, and her vital signs were within normal parameters. During her hospitalization, the patient showed no evidence of systemic compromise and was discharged 12 days after admission, with outpatient follow-up visits every 7 days to evaluate the wound. Ultimately, the lesion showed a favorable outcome with complete healing in 4 weeks with a residual scar (Fig. 10).
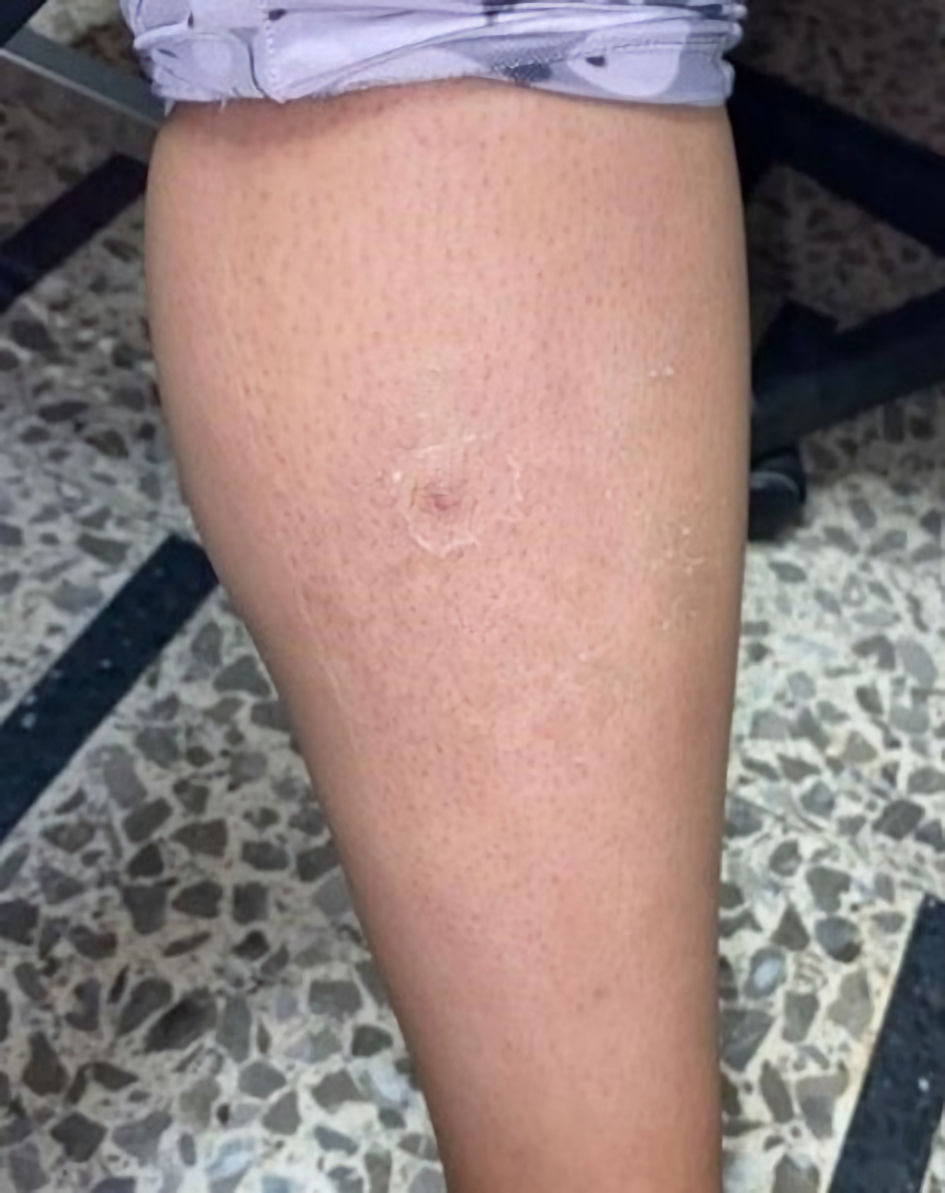 Click for large image | Figure 10. Complete resolution of the lesion 4 weeks after the attack, with residual scar. |
| Discussion | ▴Top |
Early diagnosis and treatment of loxoscelism remains a challenge in both high and low prevalence areas due to the difficulty of capturing and preserving the spider and the difficulty of rapid access to medical services. In many cases of loxoscelism, only a photograph of the spider was taken, in other cases the spider was observed only after it had attacked and fled, or in other cases the spider was never identified. The present manuscript reports three clinical cases of loxoscelism. Although in case 1 the patient developed more extensive damage to the skin surrounding the bite site, all cases ultimately showed satisfactory improvement, achieving remission of symptoms and complete healing of the wound after general therapeutic management and treatment with the fabotherapeutic Reclusmyn®.
The toxic and dermonecrotic visceral damage are produced by the coagulant, hemolytic and vasculitic necrotizing properties of the spider venom, with sphingomyelinase being its most toxic component, responsible for neutrophil activation and alteration of the complement system, causing the various presentations of loxoscelism. The most common form is the cutaneous loxoscelism (83% of cases), followed by the cutaneous-visceral form (16% of cases), with a mortality rate of 1-3%, in which the venom enters the bloodstream, causing hemolytic alterations, with consequent involvement of several organs [11, 15, 16]. Several studies have correlated the presence and severity of loxoscelism with patient characteristics such as age, sex, bite site, comorbidities, immune system, and others [1, 7, 11, 12, 16-18]. Some reports indicate that infants, adolescents, and the elderly are the groups with the most severe loxoscelism [1]. This was observed in the present manuscript where the patient in case 1 was a 14-year-old patient. It is very possible that newborns, infants, and elderly patients are the most affected in loxoscelism due to immaturity and/or decreased immune system. However, in the adolescent group, the reason for their greater susceptibility is not clear. In this sense, a recent study reported six adolescents with acute hemolytic anemia from presumed Loxosceles reclusa bites [19]. It has been described that children with loxoscelism may be more prone to hematologic complications than adults [19]. Therefore, further studies in adolescents are needed to elucidate the probable greater involvement in cases of severe loxoscelism.
Regarding gender, some reports indicate a higher prevalence of loxoscelism in women due to their greater involvement in the domestic environment. However, other studies find no significant difference in the prevalence of loxoscelism between men and women [1, 12, 13]. On the other hand, reports in the literature indicate that the upper or lower extremities, face, neck, and thorax are the most common sites of Loxosceles spider bites [1, 12, 13, 20]. This greater predilection of bite sites occurs by chance or coincidence. In the present manuscript, the bites were on the lower extremities in two cases and on the upper extremity in one case. Therefore, it is widely recommended to check the objects that people touch, to shake clothes and bedding before use, and to constantly clean and move furniture. An increased risk of systemic manifestations has been observed in thoracic bites, in patients of extreme age, and in those who present nausea, vomiting, and fever in the first hours after the attack [21], although some reports contradict this association [1, 13]. In the present manuscript, all patients presented nausea and vomiting during the first days after the attacks. However, no patient presented fever.
Identification of the lesions depends on the time elapsed between the spider bite and the evaluation of the patient. The first dermal manifestations that appear are edema and erythema, followed by violaceous coloration, induration of the lesion and increase in edema with the peculiar characteristic of gravitational distribution, forming the liveloid plaque. About 20 - 30 h after intoxication, vesicles may appear, sometimes with serohematous content, with their subsequent rupture, evolving into the central necrotic zone, forming a black eschar that, when detached, causes an ulcer of variable depth. Depending on the patient, complete healing may occur in 6 - 8 weeks [11-14, 22]. The components of Loxosceles spider venom include various proteins and peptide toxins. However, phospholipase D or sphingomyelinase D toxin is the major cause of skin necrosis and hemolysis in patients with loxoscelism [1, 2, 23, 24]. Several factors have been associated with the progression of skin necrosis, such as the amount of venom inoculated, the crushing of the spider at the time of the bite, and the characteristics of the spider itself (species, sex, and ontogenetic stage) [1, 2, 7, 23, 24]. In the present manuscript, patients in clinical cases 2 and 3 presented with mild to moderate skin lesions. However, the patient in clinical case 1 had a severe and extensive skin lesion with a large necrotic area with irregular borders, hyperpigmented, surrounding vitalized tissue, which required cleansing and surgical debridement. Fortunately, with autograft placement and local wound care, the injury healed, leaving only an atrophic scar with no other sequelae.
There are a variety of treatments for the different presentations of loxoscelism, such as the use of dapsone (a polymorphonuclear leukocyte inhibitor drug), corticosteroids, analgesics, antihistamines, antibiotics, anticoagulants, and others. However, none of these are specific for Loxosceles spiders. The use of dapsone is also limited to cases of cutaneous loxoscelism due to its side effects related to the production of hemolysis and methemoglobinemia [11, 12, 25]. Several antisera, or antivenoms, have been developed for Loxosceles spider venom. In general, antivenoms consist of fractions or components of IgG from the plasma of animals hyperimmunized with spider venom. Some antivenoms are being developed and marketed in various countries such as Mexico, Peru, and Brazil [11, 12, 26, 27]. Anti-Loxosceles serum reduces the severity of skin lesions in animal models and in clinical situations [26, 28]. In this sense, administration of polyvalent anti-arachnid antivenom to 74 patients with cutaneous loxoscelism reduced the likelihood of developing necrosis, and also reduced the depth of the ulcers that subsequently developed [28]. Reclusmyn® antivenom (developed and commercialized in Mexico) is a polyvalent fabotherapeutic specific for spiders of the genus Loxosceles sp. It is a compound derived from horse plasma hyperimmunized with necrotic toxins of the species Loxosceles laeta, Loxosceles boneti and Loxosceles reclusa [26, 27]. This fabotherapeutic drug has been used in Mexican patients with cutaneous loxoscelism and systemic loxoscelism, showing beneficial effects [22]. In our manuscript, all patients received Reclusmyn® antivenom and had favorable responses with complete remission of systemic symptoms and healing of the skin lesion. It is important to note that the patients in cases 1 and 3 started antivenom early (3.5 h and 22 h, respectively). Only the patient in case 2 did not start antivenom administration until approximately 144 h after the attack. Previous reports have mentioned a better efficacy of antivenom when administered in the first 72 - 120 h after the spider bite [26, 28, 29]. However, other reports indicate that antivenom can be administered within 7 to 10 days after the attack [22, 27]. In this sense, more studies are needed to evaluate the efficacy of antivenom in different clinical circumstances and over different periods of time. Treatment of the skin lesion caused by the spider bite involves local cold, elevation of the affected limb, cleaning of the lesions and extraction of the necrotic fragments. For deep and extensive injuries, grafting may be performed for adequate healing [29]. Another alternative treatment is the use of negative pressure, which, along with the use of silver or collagen dressings, can increase the development of granulation tissue [29, 30].
The limitation we faced in this report was the lack of identification of the specimen associated with the bite in two of the case reports. However, the probable diagnoses were made mainly by the characteristics of the skin lesions, the history of feeling a type of bite, and its clinical evolution. In our country, the reporting of cases related to Loxosceles envenoming is scarce because it is not a pathology that must be reported according to our laws and regulations, so there are few statistics on the subject, and the real incidence of this envenomation is unknown [5, 7].
Conclusions
Human contact with a venomous animal (of the classes Arachnida, Amphibia, Reptilia, Cephalopoda or Cubozoa) should be considered a medical emergency requiring rapid initiation of treatment with general measures and the appropriate antivenom. The above may delay, reduce, or prevent damage to the site of contact (skin and mucous membranes) and probable damage to other organs and systems. In our study, early treatment with antivenom prevented or reduced the systemic manifestations of Loxosceles spider envenomation in two of our cases, and in another patient after 7 days. The indication for treatment with antivenom is in cases of documented, probable or presumptive loxoscelism, taking into account the identification or not of the spider, the type of skin lesion and the clinical evolution of the patient. The dosage regimen, which includes the number of doses and the intervals between doses, is recommended by the developer and marketer of the polyvalent anti-Loxosceles fabotherapeutic (Reclusmyn®) and is based on the time elapsed since the spider bite, the age of the patient, and the clinical evolution of the patient [27]. In our country, there are no official guidelines for the treatment of loxoscelism. Therefore, it is of utmost importance to increase research on this pathology, in order to establish evidence-based treatment guidelines for its management and prevention, as well as to provide updated and concrete information to healthcare professionals to help them make a correct diagnosis and apply the best therapy adapted to the needs of each patient.
Learning points
Loxosceles spider bites can cause loxoscelism, which can be systemic-visceral or cutaneous. Early diagnosis of loxoscelism is challenging due to the difficulty of capturing and preserving the spider. Treatment of a Loxosceles spider bite includes application of local cold, rest, elevation of the extremity (if possible), antihistamines, corticosteroids, antibiotics, dapsone, non-steroidal anti-inflammatory drugs, Loxosceles antivenom, and care of the skin lesion until it heals. Cases of cutaneous loxoscelism should always be monitored for possible progression to systemic loxoscelism, which can be fatal.
Acknowledgments
None to declare.
Financial Disclosure
The authors of this publication do not have any relevant financial disclosure.
Conflict of Interest
None to declare.
Informed Consent
Regarding the ethical aspects, the Declaration of Helsinki was followed in the three clinical cases, protecting the privacy and confidentiality of the patients in the study. Written consent was obtained from the patients for the use of their clinical cases and photographic images of the evolution of the lesions produced by the spider bite.
Author Contributions
Omar Azuara-Antonio, MD, conceptualization (lead), data curation (lead), formal analysis (lead), investigation (lead), methodology (lead), software (equal), supervision (lead), validation (lead), visualization (lead), writing-original draft (lead), writing-review and editing (lead). Mario I. Ortiz, MD, PhD, conceptualization (lead), data curation (lead), formal analysis (lead), investigation (lead), methodology (lead), project administration (lead), resources (equal), software (lead), supervision (lead), validation (lead), visualization (lead), writing - original draft (lead), writing - review and editing (lead). Karla D. Jimenez-Oliver, MD, formal analysis (equal), investigation (equal), methodology (equal), writing - original draft (equal), writing - review and editing (equal). Luis E. Hernandez-Cruz, MD, formal analysis (equal), investigation (equal), methodology (equal), writing - original draft (equal), writing - review and editing (equal). Gamaliel Rivero-Veras, MD, formal analysis (equal), investigation (equal), methodology (equal), writing - original draft (equal), writing - review and editing (equal). Luz Hernandez-Ramirez, MD, formal analysis (equal), investigation (equal), methodology (equal), writing - original draft (equal), writing - review and editing (equal).
Data Availability
The data supporting the findings of this study are available from the corresponding author upon reasonable request.
| References | ▴Top |
- Gremski LH, da Justa HC, Polli NLC, Schluga PHC, Theodoro JL, Wille ACM, Senff-Ribeiro A, et al. Systemic loxoscelism, less frequent but more deadly: the involvement of phospholipases D in the pathophysiology of envenomation. Toxins (Basel). 2022;15(1):17.
doi pubmed pmc - Oliveira-Mendes BBR, Chatzaki M, Sales-Medina DF, Leal HG, van der Veer R, Biscoto GL, Goncalves PM, et al. From taxonomy to molecular characterization of brown spider venom: An overview focused on Loxosceles similis. Toxicon. 2020;173:5-19.
doi pubmed - World Spider Catalog. World Spider Catalog. Version 24.5 Natural History Museum Bern. 2023. online at http://wsc.nmbe.ch (Accessed April 21, 2023).
doi - Navarro-Rodriguez CI, Valdez-Mondragon A. Description of a new species of Loxosceles Heineken & Lowe (Araneae, Sicariidae) recluse spiders from Hidalgo, Mexico, under integrative taxonomy: morphological and DNA barcoding data (CO1 + ITS2). Eur J Taxonomy. 2020;704:1-30.
doi - Orozco-Gil M, Desales Lara MA. Las aranas (Arachnida: Araneae) del estado - de Hidalgo, Mexico: contribucion al conocimiento de su biodiversidad. Acta Zoologica Mex. 2021;37:1-23.
doi - Zuniga-Carrasco IR, Caro-Lozano J. Aspectos clinicos y epidemiologicos de la mordedura de aranas en Mexico. Hosp Med Clin Manag. 2018;11:191-203.
doi - Sams HH, Dunnick CA, Smith ML, King LE, Jr. Necrotic arachnidism. J Am Acad Dermatol. 2001;44(4):561-573.
doi pubmed - Hurtado VJ, Sotelo CN, Ibarra SR. Envenenamiento por Loxosceles reclusa (arana “parda”). Rev Mex Ped. 2005;72:85-88
- Nguyen N, Pandey M. Loxoscelism: cutaneous and hematologic manifestations. Adv Hematol. 2019;2019:4091278.
doi pubmed pmc - Jacobs JW, Bastarache L, Thompson MA. Laboratory Predictors of Hemolytic Anemia in Patients With Systemic Loxoscelism. Am J Clin Pathol. 2022;157(4):566-572.
doi pubmed - Manriquez JJ, Silva S. [Cutaneous and visceral loxoscelism: a systematic review]. Rev Chilena Infectol. 2009;26(5):420-432.
pubmed - Lopes PH, Squaiella-Baptistao CC, Marques MOT, Tambourgi DV. Clinical aspects, diagnosis and management of Loxosceles spider envenomation: literature and case review. Arch Toxicol. 2020;94(5):1461-1477.
doi pubmed - Droppelmann K, Majluf-Caceres P, Sabatini-Ugarte N, Valle E, Herrera H, Acuna D. Loxoscelism. experience in 200 patients. Rev Med Chil. 2021;149(5):682-688.
doi pubmed - Puerto CD, Saldias-Fuentes C, Curi M, Downey C, Andino-Navarrete R. [Experience in visceral cutaneous and cutaneous loxoscelism of hospital management: clinical, evolution and therapeutic proposal]. Rev Chilena Infectol. 2018;35(3):266-275.
doi pubmed - Rios JC, Perez M, Sanchez P, Bettini M, Mieres JJ, Paris E. [Prevalence and epidemiology of Loxosceles laeta bite. Analysis of consultations to a poison control center]. Rev Med Chil. 2007;135(9):1160-1165.
doi pubmed - Gremski LH, Trevisan-Silva D, Ferrer VP, Matsubara FH, Meissner GO, Wille AC, Vuitika L, et al. Recent advances in the understanding of brown spider venoms: From the biology of spiders to the molecular mechanisms of toxins. Toxicon. 2014;83:91-120.
doi pubmed - Valdez-Mondragon A, Cortez-Roldan MR, Juarez-Sanchez AR, Solis-Catalan KP, Navarro-Rodriguez CI. Aranas de importancia medica: aranas violinistas del genero Loxosceles en Mexico, que sabemos de su distribucion y biologia hasta ahora? Boletin AMXSA. 2018;2:14-24.
- Vetter RS. Spiders of the genus Loxosceles (Araneae, Sicariidae): a review of biological, medical and psychological aspects regarding envenom-ations. J Arachnology. 2008;36:150-163.
- McDade J, Aygun B, Ware RE. Brown recluse spider (Loxosceles reclusa) envenomation leading to acute hemolytic anemia in six adolescents. J Pediatr. 2010;156(1):155-157.
doi pubmed pmc - Leach J, Bassichis B, Itani K. Brown recluse spider bites to the head: three cases and a review. Ear Nose Throat J. 2004;83(7):465-470.
pubmed - da Silva PH, da Silveira RB, Appel MH, Mangili OC, Gremski W, Veiga SS. Brown spiders and loxoscelism. Toxicon. 2004;44(7):693-709.
doi pubmed - Moranchel-Garcia L, Pineda-Galindo LF, Casarrubias-Ramirez M, Mendoza-Alvarez SA, Olvera-Acevedo A, Alfaro-Mejia JA, Iniestra-Flores F, et al. Evolucion clinica de pacientes con loxoscelismo sistemico y dermonecrotico en un hospital de tercer nivel. Med Int Mex. 2017;33:18-27.
- McGlasson DL, Harroff HH, Sutton J, Dick E, Elston DM. Cutaneous and systemic effects of varying doses of brown recluse spider venom in a rabbit model. Clin Lab Sci. 2007;20(2):99-105.
pubmed - de Oliveira KC, Goncalves de Andrade RM, Piazza RM, Ferreira JM, Jr., van den Berg CW, Tambourgi DV. Variations in Loxosceles spider venom composition and toxicity contribute to the severity of envenomation. Toxicon. 2005;45(4):421-429.
doi pubmed - Ghaoui N, Hanna E, Abbas O, Kibbi AG, Kurban M. Update on the use of dapsone in dermatology. Int J Dermatol. 2020;59(7):787-795.
doi pubmed - Isbister GK, Graudins A, White J, Warrell D. Antivenom treatment in arachnidism. J Toxicol Clin Toxicol. 2003;41(3):291-300.
doi pubmed - Instituto Bioclon. Faboterapia. Guia de tratamiento en intoxicaciones por animales ponzonosos. Available from: https://seciss.facmed.unam.mx/wp-content/uploads/2022/03/guia-de-tratamiento-2014.pdf.
- Malaque CMS, Novaes CTG, Piorelli RO, Risk JY, Murad JC, Lara AN, Virgulino CC, et al. Impact of antivenom administration on the evolution of cutaneous lesions in loxoscelism: A prospective observational study. PLoS Negl Trop Dis. 2022;16(10):e0010842.
doi pubmed pmc - Menendez A, Ordaz Cortes R. Uso de terapia VAC(r) para tratamiento de heridas por mordedura de arana reclusa cafe. Cir Plast Iberolatinoam. 2011;37:295-298.
doi - Anderson J, Hanson D, Langemo D, Hunter S, Thompson P. Atypical wounds: recognizing and treating the uncommon. Adv Skin Wound Care. 2005;18(9):466-470.
doi pubmed
This article is distributed under the terms of the Creative Commons Attribution Non-Commercial 4.0 International License, which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
Journal of Medical Cases is published by Elmer Press Inc.


